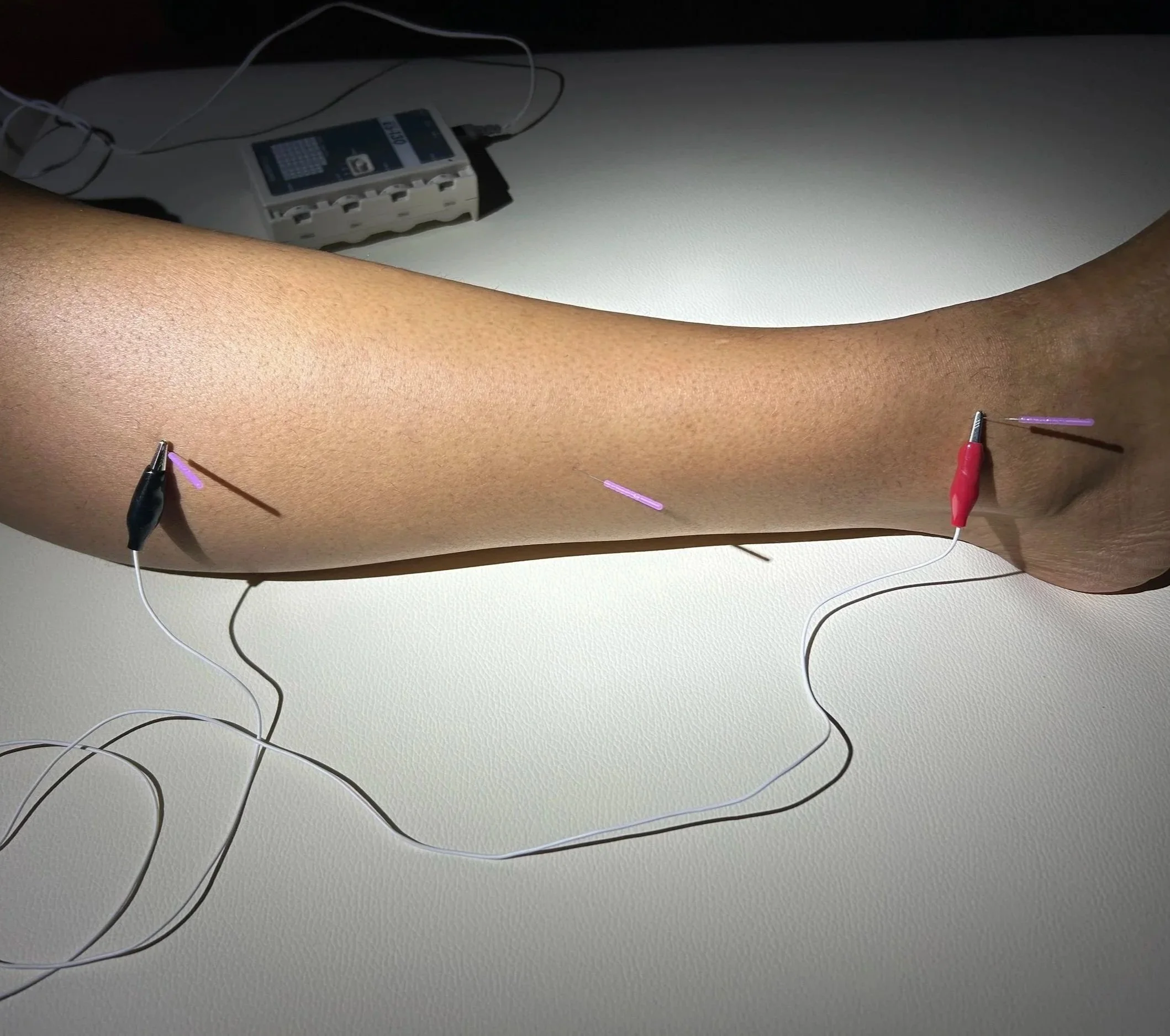
Dry Needling
A 30 min Dry needling session uses needles as thin as one of your hair , consistently over a period of time to address tissue restrictions in the body.
Dry needling is a skilled, research‑informed technique that uses very thin, solid needles to release tension and irritation in muscles, fascia, and the nervous system. By targeting myofascial trigger points and specific neuro‑fascial pathways, this approach helps reduce pain, improve joint mobility (such as ankle dorsiflexion), and restore ease of movement in areas like the low back, hips, and legs. Because the fascia and nervous system are continuous from head to toe, strategic “neuro dry needling” can also influence distant regions and the brain’s body map (homunculus), supporting better coordination, balance, and functional mobility even when neuropathy or chronic pain are present.
In post‑stroke hemiplegia, dry needling of spastic or myofascial‑restricted muscles provides not only local biomechanical benefits but also powerful somatosensory input into the damaged hemisphere’s body map (homunculus). Randomized and controlled studies show that adding dry needling to conventional neurorehabilitation reduces spasticity, improves limb kinematics, and enhances upper‑ and lower‑extremity function compared with therapy alone, indicating effects that extend beyond the immediate needle site. fMRI and neurophysiology data further demonstrate that dry needling can increase activation in ipsilesional primary motor and somatosensory cortices and modulate cortical excitability, supporting neuroplastic reorganization of the hemiplegic limb representation when needling is combined with task‑specific training. This provides a plausible mechanistic basis for using strategically placed, sometimes distant dry needling points (e.g., proximal limb or trunk muscles) to influence distal motor control and functional recovery in hemiplegic patients through coordinated neuro‑fascial and cortical mechanisms.
Bağcıer, F., Yurdakul, O. V., Deniz, G., Akbulut, A., Çelik, Y., & Temel, M. H. (2023). Is Dry Needling Treatment an Extra Contribution to Conventional Treatment for Hemiplegic Shoulder Pain? A Prospective, Randomized Controlled Study. Medical acupuncture, 35(5), 236–245. https://doi.org/10.1089/acu.2023.0060
Surya N, Ramamurthy G. Dry needling in stroke. Explor Neuroprot Ther. 2022;2:28–35. https://doi.org/10.37349/ent.2022.00016
A 30 min Dry needling session uses needles as thin as one of your hair , consistently over a period of time to address tissue restrictions in the body.
Dry needling is a skilled, research‑informed technique that uses very thin, solid needles to release tension and irritation in muscles, fascia, and the nervous system. By targeting myofascial trigger points and specific neuro‑fascial pathways, this approach helps reduce pain, improve joint mobility (such as ankle dorsiflexion), and restore ease of movement in areas like the low back, hips, and legs. Because the fascia and nervous system are continuous from head to toe, strategic “neuro dry needling” can also influence distant regions and the brain’s body map (homunculus), supporting better coordination, balance, and functional mobility even when neuropathy or chronic pain are present.
In post‑stroke hemiplegia, dry needling of spastic or myofascial‑restricted muscles provides not only local biomechanical benefits but also powerful somatosensory input into the damaged hemisphere’s body map (homunculus). Randomized and controlled studies show that adding dry needling to conventional neurorehabilitation reduces spasticity, improves limb kinematics, and enhances upper‑ and lower‑extremity function compared with therapy alone, indicating effects that extend beyond the immediate needle site. fMRI and neurophysiology data further demonstrate that dry needling can increase activation in ipsilesional primary motor and somatosensory cortices and modulate cortical excitability, supporting neuroplastic reorganization of the hemiplegic limb representation when needling is combined with task‑specific training. This provides a plausible mechanistic basis for using strategically placed, sometimes distant dry needling points (e.g., proximal limb or trunk muscles) to influence distal motor control and functional recovery in hemiplegic patients through coordinated neuro‑fascial and cortical mechanisms.
Bağcıer, F., Yurdakul, O. V., Deniz, G., Akbulut, A., Çelik, Y., & Temel, M. H. (2023). Is Dry Needling Treatment an Extra Contribution to Conventional Treatment for Hemiplegic Shoulder Pain? A Prospective, Randomized Controlled Study. Medical acupuncture, 35(5), 236–245. https://doi.org/10.1089/acu.2023.0060
Surya N, Ramamurthy G. Dry needling in stroke. Explor Neuroprot Ther. 2022;2:28–35. https://doi.org/10.37349/ent.2022.00016